One of the cruel ironies of fitness is that you can spend nearly all of your free time pumping iron but still be deficient in iron. If you're struggling with nagging fatigue and what feels like a never-ending cold, low iron levels could be to blame—and you've got company. Iron deficiency is the most common mineral deficiency in America, and this condition is estimated to impact more than two billion people worldwide.[1]
Are you at risk? Only testing can really say, although if you're a woman and an athlete, you're more likely to be iron-deficient. But even if you just want to hedge your bets, you owe it to yourself to be more strategic about how much iron you get in your diet, and almost as importantly, how you remove the biggest roadblocks to dietary-iron absorption.
Don't let the deficiency stats fool you. You have the ability to get your iron levels right! Find out which symptoms to look for, how to best assess your levels, and how to go about restoring them so you can restore energy and performance.
What Iron Does, Who Needs It, and How to Test
Iron is an essential mineral, meaning that your body can't produce the amount it needs to perform crucial functions. Iron is a chief component of hemoglobin, which is a protein in red blood cells responsible for transporting oxygen in the blood. Iron is also necessary for optimal growth and development of the muscular and skeletal systems, and to maintain normal cellular functioning, immune function, and synthesis of hormones and connective tissue.[1] If some of that sounds a little vague, that's just because iron does so much, in so many parts of your body, that it's hard to get across without a textbook.
So you much do you need? The recommended dietary allowance (RDA) is 8 milligrams for men and 18 mg for women, respectively.[1,2] Women have elevated needs due to iron loss that occurs during the menstrual cycle, and as a result are at a higher risk for iron deficiency compared to men. This risk is further heightened in female athletes; in fact, it's estimated that 26-60 percent of female athletes are affected by iron deficiency.[3-5]

Regardless of sex, all athletes are at risk for paltry iron stores due to iron loss in sweat. But if you do a lot of running, you're at particular risk for iron loss due to a phenomenon known as footstrike hemolysis, which is the increased breakdown of red blood cells and ultimate loss of iron due to repetitive impact against the ground.
Not having enough iron can lead to a slew of health and performance-related consequences such as chronic fatigue; frequent illness related to a compromised immune system; unpredictable changes in mood; decreased appetite; and loss of endurance, power, and desire to train. Talk about a recipe for disaster!
If you train hard and notice a recurring pattern of one of the symptoms described above, it may be worthwhile to get your iron levels tested. The gold-standard test is one that looks at serum ferritin, which reveals total iron storage within the body.[6,7]
There are other methods, but a systematic overview of the diagnostic techniques for iron-deficiency anemia showed that serum ferritin outperformed all others.[8] When discussing options with your physician, opt for this methodology if available.
Where to Get Your Iron
Iron can be found in an abundance of foods. However, not all foods contain the same type of iron.
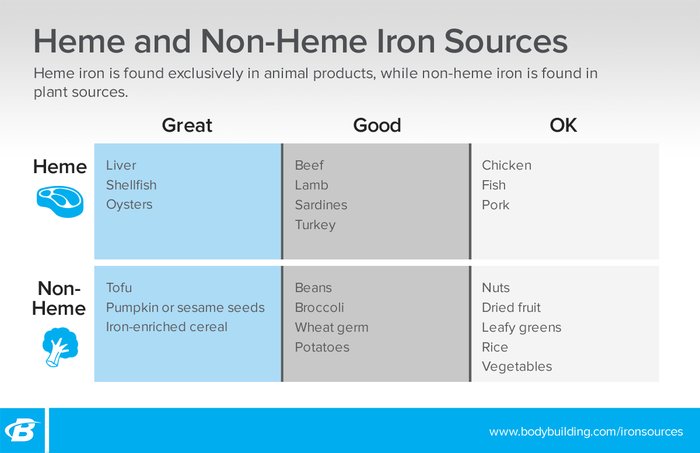
There are two forms of iron: heme and non-heme. The former is found exclusively in animal products, since it is derived from hemoglobin. The latter is found in plant sources. Your body absorbs and utilizes heme iron far more efficiently than non-heme, but this definitely doesn't mean that vegetarians are doomed to chronically low iron levels.
How to Enhance Iron Absorption
If you think your iron stores are low or a physician has confirmed that they are, don't fret. There are plenty of options you can take to boost iron levels. Make it a priority, and you might be feeling and performing better in a matter of weeks.
1. Eat Red Meat or Shellfish Twice a Week
Surf and turf, baby! Unless you're a vegetarian, this is a no-brainer. Don't like liver? Maybe you just don't know how to prepare it right. Fried chicken livers and paté both taste a lot better than that dry beef liver your grandparents may have tried to get you to eat. Don't each much shellfish? Maybe you should start.

Steak is also a solid iron source, of course. If you're concerned that eating beef twice a week will negatively impact your waistline, opt for a leaner cut such as top round, flank, sirloin, or filet.
2. Pair Iron-Rich Foods With Vitamin C
Vitamin C enhances non-heme iron absorption. It does so by preventing the formation of nonabsorbable iron compounds and preventing the reduction of ferric iron into insoluble ferrous iron.[9,10] Excellent sources of vitamin C include oranges, strawberries, kiwi, and limes.
A word of caution here, though. Spinach, although rich in vitamin C, also contains a high amount of oxalic acid, which inhibits iron absorption. Some people believe this is sufficient to block iron absorption in a meal, though there are studies indicating it's not a concern.[11]
Still, if iron is a high priority for you, consider having your nutrient-rich spinach at a different time of day.
3. Avoid Pairing Iron-Rich Foods With Dairy, Coffee, or Teas
When iron is consumed with coffee or tea, absorption rates can be decreased by as much as 35-62 percent. Given that your body only absorbs 2-20 percent of the non-heme iron you consume, any further reduction makes those sources pretty much nonexistent.
If you like to start your day with a bowl of oatmeal and fruit, consider drinking your morning cup of joe an hour before you eat. Or, save that glass of milk for bedtime rather than with your tofu stir-fry.
4. Cook With a Cast-Iron Skillet
When utilizing a cast-iron skillet to sear your steak dinner, you'll actually further boost the meal's iron content, because some of the iron from the pan is absorbed by the cut of beef. Yes, this is safe, and it occurs no matter the type of meat, grain, or veggie you use!

How much iron it ends up conveying is hard to determine, but the use of iron cookware has been a successful intervention in reducing iron deficiency in developing countries.[12]
5. Supplement the Right Way
Research suggests that supplementation is effective in improving iron status and enhancing performance.[13] However, it's important to first seek advice and testing from your physician to determine whether supplementation is appropriate for you.
A traditional women's multivitamin will provide you with the RDA of 18 milligrams per serving; however, if you have low stores, you might benefit from an iron supplement that provides closer to 30 milligrams per serving. When choosing an iron supplement, it's important to choose a supplement that ends in "-ate" such as ferrous sulfate, gluconate, and fumarate. These iron salts are absorbed best.
To optimize absorption and minimize risk of an unsettled stomach when supplementing with iron, most people benefit from taking iron on an empty stomach. However, for some people, taking iron with a small amount of food is necessary to stave off nausea.
Try both approaches, and stick with what works best for you. Be careful not to take too much at once, though, as this may lead to nausea, constipation, and GI distress.
References
- Office of Dietary Supplements - Dietary Supplement Fact Sheet: Iron. (n.d.). Retrieved August 11, 2016, from https://ods.od.nih.gov/factsheets/Iron-HealthProfessional/#h10.
- Trumbo, P., Yates, A. A., Schlicker, S., & Poos, M. (2001). Dietary reference intakes: vitamin A, vitamin K, arsenic, boron, chromium, copper, iodine, iron, manganese, molybdenum, nickel, silicon, vanadium, and zinc. Journal of the American Dietetic Association, 101(3), 294-301.
- Constantini, N. W., Eliakim, A., Zigel, L., Yaaron, M., & Falk, B. (2000). Iron status of highly active adolescents: evidence of depleted iron stores in gymnasts. International Journal of Sport Nutrition, 10(1), 62-70.
- Cowell, B. S., Rosenbloom, C. A., Skinner, R., & Summers, S. H. (2003). Policies on screening female athletes for iron deficiency in NCAA division IA institutions. International Journal of Sport Nutrition and Exercise Metabolism, 13, 277-285.
- Malczewska, J., Szczepańska, B., Stupnicki, R., & Sendecki, W. (2001). The assessment of frequency of iron deficiency in athletes from the transferrin receptor-ferritin index. International Journal of Sport Nutrition and Exercise Metabolism, 11(1), 42-52.
- Knovich, M. A., Storey, J. A., Coffman, L. G., Torti, S. V., & Torti, F. M. (2009). Ferritin for the clinician. Blood Reviews, 23(3), 95-104.
- Guyatt, G. H., Oxman, A. D., Ali, M., Willan, A., McIlroy, W., & Patterson, C. (1992). Laboratory diagnosis of iron-deficiency anemia. Journal of General Internal Medicine, 7(2), 145-153.
- Finch, C. A., Stray, S., Huebers, H. A., Bellotti, V., Lipschitz, D. A., Cook, J. D., & Pippard, M. J. (1986). Plasma ferritin determination as a diagnostic tool. Western Journal of Medicine, 145(5), 657.
- Hallberg, L., Brune, M., & Rossander, L. (1988). The role of vitamin C in iron absorption. International journal for vitamin and nutrition research. Supplement= Internationale Zeitschrift fur Vitamin-und Ernahrungsforschung. Supplement, 30, 103-108.
- Lane, D. J., & Richardson, D. R. (2014). The active role of vitamin C in mammalian iron metabolism: much more than just enhanced iron absorption! Free Radical Biology and Medicine, 75, 69-83.
- Bonsmann, S. S., Walczyk, T., Renggli, S., & Hurrell, R. F. (2008). Oxalic acid does not influence nonhaem iron absorption in humans: a comparison of kale and spinach meals. European Journal of Clinical Nutrition, 62(3), 336-341.
- Geerligs, P. D., Brabin, B. J., & Omari, A. A. A. (2003). Food prepared in iron cooking pots as an intervention for reducing iron deficiency anaemia in developing countries: a systematic review. Journal of Human Nutrition and Dietetics, 16(4), 275-281.
- DellaValle, D. M. (2013). Iron supplementation for female athletes: effects on iron status and performance outcomes. Current Sports Medicine Reports, 12(4), 234-239.

