Mike Jenkins was a big man, even among the giants who competed against him. A former college football offensive lineman, Mike tipped the scales just south of 400 pounds, carried ably on his muscular 6-foot-6 frame. Mike's specialty was strongman events, in which he held a number of international records, and his resume included a win at the 2012 Arnold Strongman Classic in Ohio. Mike was, quite simply, the physical embodiment of a Greek warrior.
Mike had something in common with another Greek warrior, a demigod named Achilles. It was, in fact, a vulnerability. To make matters worse, Mike's weakness would reveal itself only after he'd fallen asleep.
Mike suffered a fatal cardiac event on November 28, 2013, at age 31. The heart attack he suffered in his sleep may or may not have been influenced by the use of performance-enhancing drugs. What wasn't up for debate was what his wife Keri saw every night: his battle with obstructive sleep apnea (OSA), a sleep disorder that affects nearly 10 percent of the American population in moderate to severe cases, and another 10 percent in a milder form.[1] Severely overweight, middle-aged men are the classic cases, but OSA afflicts women and children, too. And now we're finding it disproportionately affects bodybuilders and powerlifters.
"Mike was having trouble sleeping and wasn't feeling well-rested," Keri told Bodybuilding.com. "He'd snore and then stop breathing for lengths of time. Many of his competitor friends relayed to Mike that they were having success with CPAP breathing devices, so Mike got tested, where it was confirmed he had obstructive sleep apnea."
In late November of last year, Mike received approval from his insurance company to get fitted for a machine. But he never got a chance to. He died in his sleep the very next night.

Strongman Mike Jenkins was diagnosed last november with obstructive sleep apnea. He died of a heart attack that same month in his sleep.
The Sounds Of Silence
No research links OSA specifically with larger male strength and physique athletes: recreational and pro bodybuilders, powerlifters, and strongmen. However, there has been a limited amount of published research done with NFL players, who tend to weigh more than the rest of us. A 2003 study found that the overall sleep apnea rate was 4-5 times higher in NFL players than males of similar ages, and an astounding 34 percent among linemen—some of whom are as heavy as Mike was.[2]
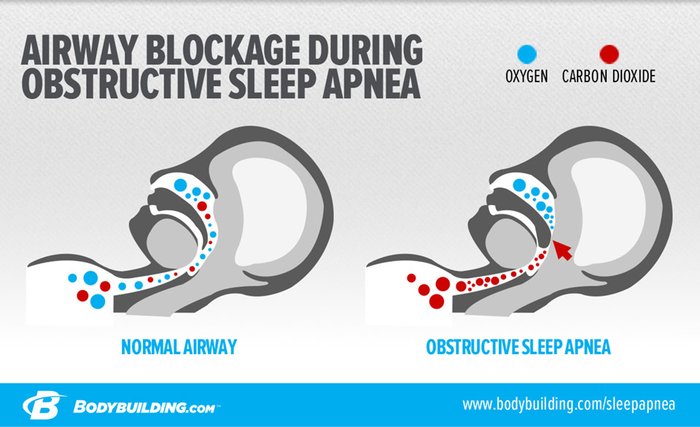
So how does OSA work? According to the American Thoracic Society, when affected individuals sleep, the soft tissues in the back of the throat begin to relax as they breathe in, ultimately collapsing back to block the throat (upper airway). That's one reason that heavy individuals who sleep on their backs typically have horrendous snoring; it's the sound of these tissues vibrating heavily during breathing. But once that airway becomes blocked, the person simply stops breathing—for 20, 30, 40, 50, 60 seconds or more—till the brain senses mortal danger and finally signals a gasp for breath.
With so little oxygen in the blood, blood pressure quickly creeps upward in the afflicted, because the heart has to work harder. Such nocturnal increases in blood pressure can lead to hypertension (chronic high blood pressure) 24/7. The risk of having a stroke or a sudden cardiac arrest soars.[3] In severe cases, OSA can trigger a heart attack in the middle of the night.
These breathless events can happen 30 or more times each hour, all night long.[4] All too often, the individual who gasps isn't fully awakened, and is completely unaware of what's going on. Often their partner will give them the first indication—by sleeping on the couch. With their sleep constantly being interrupted, individuals who suffer from OSA can go weeks, months, even years without a truly deep, restful sleep.
Fragmented sleep leads to sleepiness and chronic fatigue during the day—additional signals that OSA is hard at work while its victim tries to rest. No wonder individuals with OSA are 4-6 times more likely to be involved in a car accident, as well as be impaired on the job or suffer other medical problems, including being three times more likely to have a stroke.[5] The stealth factor is high with OSA: Symptoms may continue for years unnoticed as the person afflicted with OSA simply becomes conditioned to feeling tired all the time.
A Nightmare For Your Gains
As if the health risks aren't bad enough, OSA has another nasty surprise in store for bodybuilders: It may be robbing them of major gains. That's primarily because the natural hormones that are released endogenously by the endocrine system—yes, the muscle-building variety—are stunted when the body is unable to fully recover at night.
Test For Sleep Trouble
It's difficult to know if you have obstructive sleep apnea, but there are plenty of clues. Most of them relate to whether or not you snore, have a large neck size, your body mass index (BMI), your blood pressure, daytime fatigue levels, and other factors. Start by taking this simple questionnaire called STOP-BANG, which was developed by Dr. Frances Chung at the University Health Network, University of Toronto.[7]
You'll need to know how to compute your BMI. Divide your weight in kg by your height in meters squared. The author is 6-foot-0 and 230 pounds, so the equation would look like 104 divided by 1.83 x 1.83, or 31.05, which is below the threshold of 35.
"You're not going to get into your REM sleep because your body is not going to let you fall fully into that deep state because it has more important functions, consciously awakening you to breathe," says Guillermo Escalante, DSc, ATC, CSCS, professor of exercise science at Cal State San Bernardino and owner and fitness director of SportsPros Physical Therapy in Claremont, Calif. "That lack of deep sleep can then result in all these other hormonal issues. It could and likely does adversely affect both your testosterone and growth hormone levels." Escalante, a nationally ranked amateur bodybuilder, has suffered occasional nighttime episodes of being woken up, unable to breath, because of OSA.
According to ResMed, a global company that manufactures products for the treatment of sleep disorders, OSA has been observed since ancient times, but it wasn't until a sleep test, the polysomnograph, was developed in 1965 that it could actually be tested. Early research focused primarily on obesity—which was much more rare five decades ago than it is today—as the cause, but it became clear that obesity was not necessarily essential for OSA. Clearly, though, the two are linked. And as the national obesity pandemic has dramatically risen, so too has the incidence of OSA.
But OSA isn't just a fat person's disease. Athletes who put on significant amounts of weight are at far greater risk of getting OSA. Escalante is no fan of the Body Mass Index (BMI) because it doesn't account for the difference between muscle and fat, but in the case of OSA, the correlation with BMI is pretty clear. Extra weight and extra girth of any kind that restricts nighttime breathing seems to raise your risk. "Bodybuilders carry a lot of mass, and whether it's fat mass or lean mass, it's going to create a lot more pressure on organs and increase the demand for oxygen."
Individuals with a neck size of 17 or larger are particularly highly correlated with OSA.[6] Some 80-90 percent of individuals with the condition aren't diagnosed, so they're completely unaware they have it.[1] It's thought that the musculature of the neck encroaches on the diameter of the windpipe, so when those very same muscles that make for a thick neck begin to relax at night, they collapse on the airway.
If you're at high risk for OSA, getting your sleep assessed is the next step. Coordinate with a sleep center (many are covered by health insurance) for an overnight stay (cost about $1,100), where they wire you up and assess your condition. Take-home portable sleep monitors were recently approved by the American College of Physicians as a reliable alternative to spending the night at a sleep center, at a fraction of the cost.
Essentially the test will examine your respiration, when and how often you stop breathing, blood oxygen and carbon dioxide levels, your heart rhythm and brainwave activity, and other data. You may have a mild case of OSA (defined as 5-15 instances of stopped breathing for 10 seconds or longer each hour), or a more severe case. That assessment will determine your treatment.
Treating The Problem
There are a number of easy steps you can take for a mild case: Rinse your sinuses each night with saline to help open them up, use a nasal decongestant, sleep on your side, eliminate alcohol before going to bed, and use a nasal strip to help open your airways. Certainly losing a few pounds can help, too.
Treatment for more severe cases might include:
- Inserting a custom-made mouthpiece during sleep that essentially pulls the lower jaw forward to keep the airway open.
- Surgery to remove tissue in the back of the mouth and open up constricted airway passages, though this treatment is not always successful and reportedly very painful.
- Using an assisted breathing machine with continuous positive airway pressure (CPAP), which is the most widely used treatment for moderate to severe OSA according to the American Academy of Sleep Medicine. A small compressor blows air into a mask worn snugly over your nose and mouth during sleep. The pressure acts like a splint, keeping the airway continuously open, preventing apnea and snoring.
Of note, treating the symptoms of sleep apnea—for example by taking blood pressure medicine to help control hypertension—has been shown in research to be ineffective, reported the AASM just recently.[8] Only by treating the problem—OSA—can you directly improve high blood pressure.

CPAP And The Bodybuilder
No doubt you're thinking how decidedly unsexy you're going to look at night hooked up to a machine with a breathing tube. It may well be uncomfortable, make you feel claustrophobic, and even leave your mouth dry. You might also be embarrassed to wear it in front of others. Those are just a few of the reasons why the compliance rate for individuals who are diagnosed with OSA and have CPAP machines is so low.
Studies have shown the compliance rate of using CPAP machines at just 29-83 percent, depending on the study.[9,10] Compliance rates in the limited number of studies have been all over the map, so it's hard to even venture a guess as to how many people even use their CPAP. Many individuals never actually don the apparatus after purchasing one.
You could lose weight and try to remedy the underlying condition, and for the vast majority of people, that would be ideal. But some bodybuilders and powerlifters don't want to get smaller, even when it's clear that their size is causing OSA. Oftentimes a bodybuilder will find that when preparing for a competition—when his bodyweight drops significantly—his nighttime breathing improves. It gets worse again when he goes back to an "offseason" weight.
Not surprisingly, then, many bodybuilders who don't want to quit their vocation ultimately chose to use a CPAP device.
The research on OSA and strength athletes may be lacking, but the anecdotal evidence has been mounting fast. I have known a number of recreational bodybuilders—not even pros, mind you—who reveal symptoms of OSA. I've had symptoms myself, but I didn't take my sleep issues seriously until I spoke with Carl Cheung, a Canadian bodybuilder.

The research on OSA and strength athletes may be lacking, but the anecdotal evidence has been mounting fast. I have known a number of recreational bodybuilders—not even pros, mind you—who reveal symptoms of OSA.
Cheung, an amateur bodybuilder from Mississauga, Ontario, who competed in the Canadian Nationals on September 6, was alerted to his condition by a girlfriend six years ago. His doctor, Cheung said, was surprised he was still alive—his condition was that bad. He was tested and the results showed that he woke up more than 300 times, including one instance in which he stopped breathing for four full minutes.
Cheung, now 35, overcame his initial fears and embarrassment about using a CPAP device. He lists a number of ways the machine has improved his quality of life.
"I've been using [the CPAP machine] since 2008 and I'm no longer extremely fatigued. I can now remain focused during work meetings. I have faster reaction times driving and no longer fall asleep at a red light. I actually require less sleep than before because I'm getting a better quality of sleep. Physically I was able to lose body fat easier and sustain quality muscle mass. My appetite has increased. My blood pressure went down. I experienced a better mood and felt less frustration because I was no longer constantly exhausted. I even have a better sex drive because my hormones improved based on consistent, quality sleep."
The good news isn't just anecdotal. Research shows that individuals who stick with CPAP treatment show a reduction in apnea, consistently feel better, and encounter fewer complications of the disease.[11] The CPAP machine also eliminates snoring.
Compounding The Problem
Ironically for bodybuilders like Cheung, the use of CPAP has enabled them to make further gains in size and strength, gains they might otherwise not have been able to achieve. Without the device, such gains in weight could further compound their nighttime breathing issues.
"It's kind of like a whole-circle effect," says Escalante. "You're a big guy trying to gain more mass, and now you put this machine on and it facilitates your ability to get bigger because your hormones are working more efficiently. That can make the breathing problem even worse."
For now, Cheung has found a solution. "Each time I've made permanent gains I'm required to get retested and make necessary adjustments to the device to compensate for the amount of oxygen required to support the larger mass," he says.

The use of CPAP has enabled bodybuilders to make further gains in size and strength, gains they might otherwise not have been able to achieve. Without the device, such gains in weight could further compound their nighttime breathing issues.
Ending The Nightmare
The irony that the biggest men in bodybuilding are required to use CPAP machines just to survive isn't lost on Escalante. "Bodybuilding is such an extreme sport and we're pushing our physiological limits," he says. "At that point there are going to be certain systems in our bodies that are going to need some help. Because we're pushing those physiological limits, I think you're going to see some of these shortfalls in which your body is just saying, 'You know what, I wasn't meant to handle that and I need some help.'"
Clearly, a dearth of research among bodybuilders and strength athletes isn't helping. "I think this would be a critical area for research that's been sorely lacking to get some valid information and see how many people from our sport and other sports where size is important, to see how many people are suffering from it," he adds. "I don't think there's much education going on either. Hopefully we'll start to open up some eyes."
Today, everything is supersized—including the bodybuilders, powerlifters, strongmen, and NFL and college players who dominate competitive sports. But as these men test their physical limits, unforeseen dangers that were previously unknown have arisen along with their bodyweight, in part because evolution has not kept up with their gains in size. For some, it may well be an airway blockage that makes every breath at night a struggle for survival.
Author's note: My sincere thanks to Keri Jenkins, who has found the courage to share Mike's story in hopes that it will help other men get tested and treat their condition.
References
- Medline Plus/ScoutNews. Portable Monitors OK For Spotting Sleep Apnea: New Guidelines, August 2014.http://m.medlineplus.gov/news/fullstory_147684.htm
- George C, Kab V, Levy A. Increased Prevalence Of Sleep-Disordered Breathing Among Professional Football Players, New England Journal Of Medicine. 348:367-368. 23 Jan. 2003.
- Rowley JA, McGowen C, Lareau S, Fahy B, Garvey C, Sockrider M. What Is Obstructive Sleep Apnea In Adults, Patient Information Series, American Thoracic Society, 2009.
- Sleep Apnea. American Academy of Family Physicians, May 2014.
- Statistics & Research. http://www.midwestapnea.com/statistics--research.html. 3 Sept. 2014.
- Schmidt-Nowara Wolfgang. Patient Information: Sleep Apnea In Adults (Beyond The Basics), Wolters Kluwer (UpToDate.com), July 2014.
- The STOP-BANG questionnaire is the property of the University Health Network at the University of Toronto. Reprinted with permission.
- American Academy Of Sleep Medicine. Severity Of Sleep Apnea Impacts Risk Of Resistant High Blood Pressure, 14 Aug. 2014. Aasmnet.org Web. 15 Aug. 2014.
- Weaver TE, Kribbs, NB, Pack Al, et al. Night-To-Night Variability In CPAP Use Over The First Three Months Of Treatment. Sleep 1997: 20:278.
- Weaver, TE, Grunstein RR. Adherence To Continuous Positive Airway Pressure Therapy: The Challenge To Effective Treatment. Proc Am Thorac Soc 2008; 5:173.
- National Heart, Lung, and Blood Institute. What Is Sleep Apnea? http://www.nhlbi.nih.gov/health/health-topics/topics/sleepapnea/livingwith.html 3 Sept. 2014.

