There's no need to hit you with the stats here. You know by now that type 2 diabetes is becoming more prevalent all the time, across all age ranges, in the United States and around the world. And while preventing new cases of type 2 diabetes is rightfully a high priority for policymakers and physicians, there are crucial questions that often get overlooked in the focus on new cases.
If you're currently living with diabetes, what can you do to improve your quality of life? What steps can you take to prevent the types of cardiovascular and neurological diseases that often accompany diabetes—and ultimately lead to many early deaths?
It turns out there's a lot you can do, and not all of it has to do with what you eat. The types of activity in your life also matter immensely. And while cardiovascular training often forms the centerpiece of what diabetics and their doctors consider "exercise," there's a strong, research-backed case to be made that resistance training should be just as central to your approach.
Here's why you need to pick up a weight, and what you need to know to start!
Diabetes And Exercise
Physical activity is known to be a remarkably effective tool to help manage type 2 diabetes. In fact, along with dietary choices, it's as effective as any medication a doctor can give you.[1]
Exercise is great for a number of reasons, but first in line for diabetics is its ability to promote healthy blood glucose values (or the amount of sugar circulating in your bloodstream) and improve insulin sensitivity, which refers to the ability of the hormone insulin to usher that sugar (glucose) out of your bloodstream and into cells.[2-3]

Resistance training has been shown to provide benefits for diabetics above and beyond aerobic-based training approaches alone.
But what kind of exercise works best? Aerobic exercise is a great tool for improving cardiovascular health, of course, which is important because most people who have type 2 diabetes are at greater risk for cardiovascular complications. However, resistance training has been shown to provide benefits for diabetics above and beyond aerobic-based training approaches alone.
These benefits include:
- Overall control of blood glucose levels, both in younger and older populations[4-6]
- A stabilized blood glucose response that lasts longer post-exercise than aerobic training alone[7]
- Improved body composition, or in layman's terms, more muscle and less fat. Obesity is a risk factor for many complications that often accompany type 2 diabetes. The more muscle you have, the more calories you burn at rest, and the more activity you can undertake in your life
- Improvements to a number of other important health markers, such as cholesterol profiles[2,3,7,8]
- Increased muscle mass, which is tied to a longer life expectancy—more, in fact, than the popular standard of "body-mass index," or BMI[9]
It's not a stretch to say that if you are diabetic, you need to strength train—probably even more than nondiabetics, in fact. It can not only help you manage your disease, but also help you feel better, do more things you enjoy, and live longer overall.
Should I Train For Strength Or For Muscle?
Lifting weights may sound intimidating and overwhelming, especially if you're new to the pursuit. You might imagine yourself grinding through heavy, intense reps like a competitive powerlifter. While that is one way to train, it's not the ideal way for most diabetics, so don't worry about buying a powerlifting singlet just yet.
Most of the researched benefits that arise from strength training for diabetics are a result of increased muscle mass (hypertrophy), not maximum strength. Studies have linked this type of training most directly to improved measures of blood glucose and decreased risk of diabetes-related health complications, particularly in older adults.[4-6,10]
For instance, researchers out of Tufts University in 2007 demonstrated significant improvements in both muscle size and whole-body insulin sensitivity in type 2 diabetics following a hypertrophy-based program for 16 weeks.[11] In addition, hypertrophy-specific training has been shown to improve insulin sensitivity in type 2 diabetics by up to 48 percent.[12]
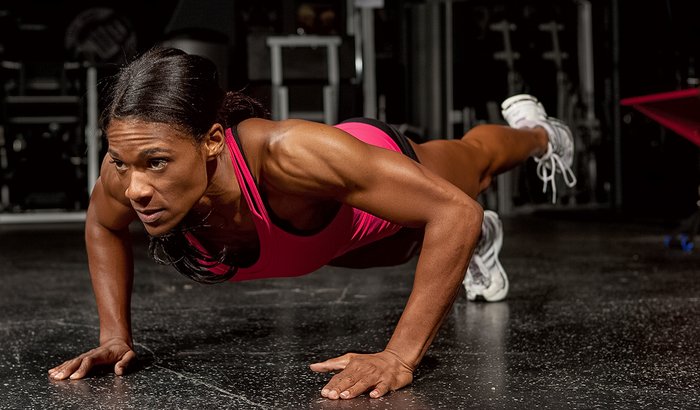
Serious lifters often schedule their training in a "split" that focuses on certain body parts each day. However, if you are primarily lifting to boost your quality of life and help manage your disease, a full-body session 2-3 times a week is probably sufficient.
Training for maximum strength can also be risky for certain diabetics. Intense, low-repetition lifting can significantly increase the risk of retinal detachment due to increases in blood pressure if you suffer from diabetic retinopathy, a microvascular complication that affects the sensitive tissues of the eye. All people with either type 1 or type 2 diabetes are at some risk of retinopathy, and the prevalence goes up dramatically over time.
This is a reason to talk with your doctor before starting strength training, but it's also a reason to do the majority of your training with slightly lighter weights at higher rep ranges. For a tried-and-true approach to hypertrophy that can be scaled for ability, do 1-2 warm-up sets with light weight, then 3-4 working sets of 8-12 reps for each major muscle group. The last couple of reps in each set should be a struggle.
Serious lifters often schedule their training in a "split" that focuses on certain body parts each day. However, if you are primarily lifting to boost your quality of life and help manage your disease, a full-body session 2-3 times a week is probably sufficient.
Here's an example of how it could look:



BodyFit
$6.99/month- 2,500+ expert-created single workouts
- 3,500+ how-to exercise videos
- Detailed workout instruction
- Step-by-step workout tips
- Training at gym or at home
- Access to Workout Plans
- Access to Bodyfit App
- Store Discounts
Already have a Bodybuilding.com account with BodyFit? Sign In

What comes with BodyFit?

- Instructional Videos
Don't risk doing a workout improperly! Avoid injury and keep your form in check with in-depth instructional videos.

- How-to Images
View our enormous library of workout photos and see exactly how each exercise should be done before you give it a shot.
- Step-by-Step Instructions
Quickly read through our step-by-step directions to ensure you're doing each workout correctly the first time, every time.
As you become more proficient and begin to use heavier weights, you can add exercises or undertake a more complex program.
What About Cardio?
The current recommendations from the American Diabetes Association (ADA) and American College of Sports Medicine (ACSM) suggest diabetics accumulate a minimum of 150 minutes of moderate-to-vigorous aerobic exercise spread throughout the week.[13,14] Especially alongside strength training, this approach can do a lot to help you improve body composition and control blood sugar levels.
But the research also indicates that you should turn up the intensity some of the time as well. In fact, while moderate-intensity steady-state cardio is great for improving cardiovascular health, high-intensity interval training (HIIT) can deliver most of the same health benefits with less of a time commitment.[15,16]

The current recommendations from the american diabetes association (ada) and american college of sports medicine (acsm) suggest diabetics accumulate a minimum of 150 minutes of moderate-to-vigorous aerobic exercise spread throughout the week.
Research in type 2 diabetics shows six sessions of interval training over a two-week period caused significant improvements in a range of important markers, including blood glucose concentrations and levels of the protein GLUT4, which may also positively influence insulin sensitivity.[15] Subjects performed 10 rounds of cycling for 60 seconds at 90 percent of their maximal heart rate, alternated with 60 seconds of rest between rounds. In a separate study, a single HIIT workout following the same protocol resulted in decreased blood glucose levels for 24 hours following exercise, compared to a nonexercise control group.[16]
The takeaway for you: To get the most out of your training, consider a combination of aerobic, HIIT, and resistance exercise! The three in combination may provide complementary benefits that are unachievable by aerobics or resistance alone.[2]
Here's how you could arrange your week:
- Strength training 45-60 minutes, three times per week
- Interval training 20 minutes twice per week, after strength training or on separate days
- Lower-intensity cardio 30-60 minutes, any day of the week
Just as one pill can't stabilize blood glucose and normalize health for a lifetime, consistency is the key when using exercise to maintain optimal insulin levels and improve body composition. Research has shown that the benefits that accompany training only come about when it is done consistently—as in, with no more than two days off at a time.[7,12]
But if you're going to combine aerobic with HIIT or resistance training, timing and arranging your strength and cardio sessions can be important to unlocking maximum benefits to your blood glucose levels. For instance, training's benefits in regard to glucose stabilization are most pronounced if resistance exercise precedes aerobic training.[17]
Before You Get Started
1. Be Prepared
To prevent exercise-induced hypoglycemia, make sure to carry a source of fast-acting carbohydrates, like a piece of fruit or a sports drink, to use as needed, especially for type 1 diabetics. Exercising with a partner is advised, to reduce the risk of blood-glucose-related problems.
2. Know Your Numbers Beforehand
Most exercises will have a relatively consistent effect on blood glucose, but it's important to know your numbers going into a workout, especially if you're starting a new program.
It's generally recommended that you refrain from any form of physical activity if your pre-exercise blood glucose levels are higher than 250 mg/dL when ketosis is present. Train with caution if your blood glucose is above 300 mg/dL without ketosis, and avoid intense exercise at this time.[18]
Conversely, if your blood glucose levels are below 100 mg/dL, it's wise to consume carbohydrates and recheck your blood glucose before starting exercise.
3. Monitor Insulin Levels Post-Workout
Type 1 diabetics may have to drastically decrease insulin-pump settings or even remove the pump during exercise to get the greatest blood-sugar-stabilization response. After training, insulin levels may need to be decreased for up to 12 hours to avoid hypoglycemia.[17] In both cases, talk to your doctor to guide your approach.
Similarly, those with type 2 diabetes should be aware that insulin utilization will improve with exercise over time, but will vary with muscle activation, type, and intensity of exercise. You may not always see the same blood glucose response depending on the workout, but that doesn't mean you're doing something wrong. Remember, long-term consistency is what will pay off the most!
Final Considerations
Before starting or modifying a current exercise program, make sure to consult with your physician. Keep in mind the following:
- All resistance and aerobic training is discouraged if your blood glucose is extremely high or low.[17]
- It's wise to avoid exercise during known times of peak medication activity.
- If you see a drop in blood pressure greater than 10-20 mmHg, stop exercising for the day.
Start slow, and gradually increase the intensity. You'll have a lot to learn along the way, but as you get better at this, you're setting yourself up for a long, healthy life!
References
- Diabetes Prevention Program Research Group. (2002). Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. The New England Journal of Medicine, 346(6), 393.
- Ramalho, A. C., de Lourdes Lima, M., Nunes, F., Cambuí, Z., Barbosa, C., Andrade, A., ... & Tem*iacute;stocles, M. (2006). The effect of resistance versus aerobic training on metabolic control in patients with type-1 diabetes mellitus. Diabetes Research and Clinical Practice, 72(3), 271-276.
- Church, T. S., Blair, S. N., Cocreham, S., Johannsen, N., Johnson, W., Kramer, K., ... & Earnest, C. P. (2010). Effects of aerobic and resistance training on hemoglobin A1c levels in patients with type 2 diabetes: a randomized controlled trial. Jama, 304(20), 2253-2262.
- Dunstan, D. W., Daly, R. M., Owen, N., Jolley, D., De Courten, M., Shaw, J., & Zimmet, P. (2002). High-intensity resistance training improves glycemic control in older patients with type 2 diabetes. Diabetes Care, 25(10), 1729-1736.
- Durak, E. P., Jovanovic-Peterson, L., & Peterson, C. M. (1990). Randomized crossover study of effect of resistance training on glycemic control, muscular strength, and cholesterol in type I diabetic men. Diabetes Care, 13(10), 1039-1043.
- Eves, N. D., & Plotnikoff, R. C. (2006). Resistance training and type 2 diabetes considerations for implementation at the population level. Diabetes Care, 29(8), 1933-1941.
- Yardley, J. E., Kenny, G. P., Perkins, B. A., Riddell, M. C., Balaa, N., Malcolm, J., ... & Sigal, R. J. (2013). Resistance Versus Aerobic Exercise Acute effects on glycemia in type 1 diabetes. Diabetes Care, 36(3), 537-542.
- Bweir, S., Al-Jarrah, M., Almalty, A. M., Maayah, M., Smirnova, I. V., & Novikova, L. (1994). Resistance exercise training lowers HbAlc more than aerobic training in adults with type 2 diabetes. Diabetology and Metabolic Syndrome, 1(27), 64.
- Srikanthan, P., & Karlamangla, A. S. (2014). Muscle mass index as a predictor of longevity in older adults. The American Journal of Medicine, 127(6), 547-553.
- Eriksson, J., Taimela, S., Eriksson, K., Parviainen, S., Peltonen, J., & Kujala, U. (1997). Resistance training in the treatment of non-insulin-dependent diabetes mellitus. International Journal of Sports Medicine, 18(4), 242-246.
- Brooks, N., Layne, J. E., Gordon, P. L., Roubenoff, R., Nelson, M. E., & Castaneda-Sceppa, C. (2007). [Strength training improves muscle quality and insulin sensitivity in Hispanic older adults with type 2 diabetes](http://Strength training improves muscle quality and insulin sensitivity in Hispanic older adults with type 2 diabetes). International Journal of Medical Sciences, 4(1), 19-27.
- Ishii, T., Yamakita, T., Sato, T., Tanaka, S., & Fujii, S. (1998). Resistance training improves insulin sensitivity in NIDDM subjects without altering maximal oxygen uptake. Diabetes Care, 21(8), 1353-1355.
- Chimen, M., Kennedy, A., Nirantharakumar, K., Pang, T. T., Andrews, R., & Narendran, P. (2012). What are the health benefits of physical activity in type 1 diabetes mellitus? A literature review. Diabetologia, 55(3), 542-551.
- American College of Sports Medicine. (2014). ACSM's guidelines for exercise testing and prescription. Lippincott Williams & Wilkins.
- Little, J. P., Gillen, J. B., Percival, M. E., Safdar, A., Tarnopolsky, M. A., Punthakee, Z., ... & Gibala, M. J. (2011). Low-volume high-intensity interval training reduces hyperglycemia and increases muscle mitochondrial capacity in patients with type 2 diabetes. Journal of Applied Physiology, 111(6), 1554-1560.
- Gross, K. (2015). The acute effect of high-intensity interval training versus moderate-intensity continuous training on postprandial blood glucose regulation. The Plymouth Student Scientist, 8(2), 29-47.
- Yardley, J. E., Kenny, G. P., Perkins, B. A., Riddell, M. C., Malcolm, J., Boulay, P., ... & Sigal, R. J. (2012). Effects of performing resistance exercise before versus after aerobic exercise on glycemia in type 1 diabetes. Diabetes Care, 35(4), 669-675.
- Sigal, R. J., Kenny, G. P., Wasserman, D. H., Castaneda-Sceppa, C., & White, R. D. (2006). Physical activity/exercise and Type 2 diabetes A consensus statement from the American Diabetes Association. Diabetes Care, 29(6), 1433-1438.