
Shoulders receive the lion's share of work in the gym. Nearly all upper-body routines involve the shoulder to some extent, if only to be held fixed and motionless for the specific movement. Even during leg work, the shoulders are involved with the stacking and unstacking of plates for all the leg routines. Shoulder pain can greatly hamper any training routine and tends to require long periods of time for complete recuperation.
Severe injuries can prematurely terminate the careers of professional athletes such as baseball pitchers with rotator cuff problems. For the non-professional athlete, even minor shoulder pain can lead to disturbed sleeping patterns from the inability to find a comfortable position at night. Let's examine shoulder anatomy in sufficient detail to highlight the basis for skeletal variations that can predispose certain individuals to persistent shoulder problems , and routines for strengthening lesser-known shoulder muscles and lifting variations to minimize further trauma.
Bear in mind that severe pain, extreme muscle weakness, or inability to perform certain movements may indicate a condition requiring medical attention. Advice presented here should not serve in place of a thorough medical evaluation since certain conditions may require specialized medical intervention or even surgery.
Due to its extremely wide range of mobility, the shoulder is one of the most complex joints in the human body. Because of its unusual bone structure and large number of muscle attachments, shoulder pain can be a daunting challenge to most physicians who typically recommend merely rest and anti-inflammatory medications for weeks to months as therapy which may or may not solve the problem.
In addition, chronic degenerative changes that accumulate from repeated trauma will likely increase the frequency of shoulder problems for most individuals as they age and continue lifting. While any single article can hardly be exhaustive on the subject of shoulder issues (whole books[16,17] have been devoted to the subject), this discussion will focus on one of the more common problems that results from a combination of unlucky anatomy, undesirable lifting technique, and insufficient attention to auxiliary musculature.
The Anatomy Of The Shoulder
The shoulder is the anatomical structure that links the arm with the torso. A wide array of muscles of particular interest to bodybuilders traverse the shoulder including: pecs, lats, delts, and even the biceps. Given that the lats and delts contribute to a wide upper body desirable by bodybuilders, much attention is focused on these muscle groups and considerable stress is applied to the shoulder. Pain and discomfort can dramatically compromise nearly any weightlifting routine.
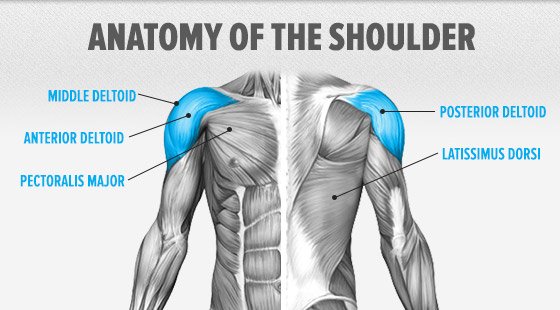
A wide array of muscles of particular interest to bodybuilders traverse the shoulder including: pecs, lats, delts, and even the biceps.
The shoulder as a joint is classically described as a ball and socket (similar in design to the hip joint).[1] The ball portion is derived from the end of the upper arm bone, the humerus, and resembles a ball stuck on the end of a long shaft, and is referred to as the humeral head. The socket side is formed from one corner of a roughly triangular flat bone called the shoulder blade (the scapula), that rests over the rib cage, high on the back and extends over the rib cage to the front of the body. The triangular form of the scapula has one side close to the midline of the back with the lower corner angling up towards the shoulder.
The third side of the triangle runs parallel to the shoulders across the top. The shoulder blade is thicker in its upper portion than the lower portion, so that the very top of the shoulder blade has a surface (rather than just as edge as with the other two sides of the triangle) with two edges (one towards the body and one away). The top edge pointing away from the body is called the spine and the surface of the top of the shoulder blade is slightly depressed and called the supraspinous fossa (fossa is the technical term for a depression). Moving along the spine towards the shoulder, a bony extension, called the acromion, juts out and arches over the top of the scapula just above the humeral head and can be felt as the bony top of the shoulder.

{{caption}}
The acromion arches over the top of the scapula from back to front and connects to the collarbone (clavicle) to complete the shoulder girdle. Arising off the top edge opposite the spine, also at the shoulder, across from where the acromion begins and pointing forward over the chest, is a small bony knob called the coracoid process. The short head of the biceps muscles attaches to this piece of bone as well as a small muscle called coracobrachialis and the pectoralis minor muscle (underneath pectoralis major, the main "pecs"). In addition, a tough ligament connects the coracoid process with the acromion.
The socket portion of the scapula that contacts the humerus is called the 'glenoid fossa,' but rather than looking like a true socket, the glenoid fossa is more open with the appearance of a saucer or rather like a golf tee with the humeral head as the golf ball. The reason for the openness is to permit a large range of motion in the joint. The downside to this large range of motion is the propensity of the shoulder to dislocate. A dislocation occurs when the humeral head moves beyond the confines of the glenoid fossa and slips over the lip of the saucer (your golf ball falls off the tee).
When any muscle acts across a joint, opposing muscles are contracted as well to stabilize the joint. Imbalances in strength between opposing muscles can potentially lead to injuries. With the shoulder, the anatomy is not as simple as a one dimensional joint (such as the elbow). Movement of the shoulder requires many different muscles to create the movement as well as other muscles to stabilize the shoulder joint. In addition, since the shoulder blade is only attached (by other bones) to the upper arm and collar bone at one end, the blade portion must be held fixed by additional muscles.
For example, serratus anterior (best seen in a well muscled, lean individual) is a small group of muscles that arises from the rib cage in front just below the pecs with the muscle bellies extending up and around to the back and disappearing underneath the lats. Serratus anterior attaches to the scapula along the edge closest to the middle of the back. Serratus's job is to prevent the shoulder blade from winging during shoulder movements; in other words, serratus pins the scapula to the back and so serves to stabilize the joint during movements.
The Rotator Cuff
As discussed above, the shoulder joint has an extremely wide range of motion. A key structure supporting the shoulder joint is the rotator cuff. The rotator cuff is concerned with two major functions, rotating the shoulder and cuffing the joint.[5,34] Rotation may not appear as an obvious movement with regard to the shoulder.
To visualize shoulder rotation, place your arm at your side and bend the elbow to 90o, as if to shake hands, but maintain the upper arm against your side and keep you palm in (thumb up).

{{caption}}
Keeping your upper arm against your side, bring your forearm and hand across your body to rest your palm on your stomach. That movement is internal shoulder rotation (the upper arm bone, the humerus, is rotating relative to the shoulder; internal is used to denote a movement towards the midline of the body). A more extreme form of internal rotation is to place the back of your hand on the small of your back, again with your elbow bent at 90°. Now keeping your elbow bent, lift your hand away from your body. One muscle of the rotator cuff, subscapularis arises from the underneath side of the shoulder blade (the side against the rib cage) and attaches to the humerus in such a way as to produce rotation of the humerus when contracted.
If the lifting of your hand away from your back produces extreme pain or is simply impossible to perform, injury to this muscle (or a tear in its tendon) may be the source. This problem requires medical attention. The opposite motion to internal rotation is external rotation (rotating your forearm away from your stomach with your upper arm against your side) and is produced by contracting two other muscles of the rotator cuff group, infraspinatus and teres minor. These muscles also arise from the shoulder blade, but on the outer side, and also attach to the humerus.
These three muscles are responsible for shoulder rotation, but the rotator cuff complex has four muscles and this is where the cuff component is involved. The fourth muscle is called supraspinatus and arises over the top of the shoulder blade (in the supraspinous fossa) and crosses the shoulder joint traveling underneath the acromion and attaching to the humerus just below the humeral head. Altogether, these four muscles (the three true rotators and supraspinatus) are the innermost set of muscles surrounding the shoulder joint and form a cuff around the joint.
Bearing in mind the shallow nature of the glenoid fossa and the propensity for the humeral head to dislocate, the contraction of all four muscles forms a tight wall around the lip of the socket to help hold the humeral head in position (centered in the glenoid fossa).[5] During almost any shoulder movement, these muscles are contracting to stabilize the joint throughout the movement by maintaining the humeral head centered in the glenoid fossa.[34]

When you throw an object, the entire movement is designed to throw your arm away from your body.
When you throw an object, the entire movement is designed to throw your arm away from your body. The object is thrown because you release your grip on it. Your arm and shoulder joint stay in place because the rotator cuff is holding the upper arm bone in place. This is why rotator cuff injuries are so devastating to baseball pitchers; a strong, intact rotator cuff is needed to allow for high velocity pitches without injuring the shoulder joint. Weakness or worse, injury to the rotator cuff can place undue stress on the shoulder joint during heavy lifting routines (because the humeral head does not stay centered in the glenoid fossa).
Strengthening the rotator cuff muscles, particularly the three involved with rotation is straightforward and basically involves movements as described above for internal and external rotation, but with light weights while lying on your side. The remaining muscle, the supraspinatus, is less straightforward and unfortunately, much advice over the years has served to compound problems, especially for those who are anatomically predisposed to have problems in the first place.[30]
Impingement Syndrome

{{caption}}
The supraspinatus muscle is involved with some of the most common causes of shoulder pain.[15] To understand its involvement and how some individuals are predisposed to suffer more than others, an appreciation of the surrounding anatomy of supraspinatus is important. As discussed above, the supraspinatus muscle arises from the roof of the scapula (shoulder blade) and attaches to the upper arm bone (humerus) on the shaft just below the humeral head. Following along the muscle's path, supraspinatus travels between the shoulder joint itself (from below) and the acromial arch (from above).
This arrangement has supraspinatus traversing a nearly complete bony tunnel with a tough ligament closing the only non-bone portion (coracoacromial ligament—connecting the coracoid process with the acromion). In addition, being part of the innermost layer of muscle would have supraspinatus moving directly on bone which is not ideal. To cushion the muscle, supraspinatus sits (and slides over) on a "bursa", a fluid filled sack that reduces friction between moving muscles and bones.
The attachment site on the humerus bone also deserves some attention. While the humerus is described as a shaft of bone with a ball-like end, bone shafts are rarely, evenly smooth across their surface. In particular, points of muscle attachments are typically raised and referred to as "tuberosities." Just below the humeral head are two such structures, the greater tuberosity, just below the acromion (on the side with your arm at your side), and the lesser tuberosity to the left in the forward direction (basically facing forward). The valley between the two tuberosities is a groove for the one of the heads of biceps' tendon to follow. Supraspinatus attaches to the upper edge of the greater tuberosity, just below the humeral head, adjacent to the biceps tendon.
The greater tuberosity has the potential to produce impingement in certain individuals who posses a specific hooked shape to their acromion.[19,23,26,29,32,33,35] In some people, the hook is exaggerated (see www.aafp.org/afp/980215ap/fongemie.html for excellent visuals). As the arm is raised (as in a side lateral raise), the greater tuberosity and acromion come quite close (they "impinge" on one another) with the bursa and the supraspinatus muscle sandwiched in between.
Compression alone can damage either the bursa (producing inflammation called bursitis, a common condition among older individuals) or the supraspinatus muscle itself (or its tendon) and is called impingement syndrome.[27] The result is pain whenever, the arm is raised since supraspinatus when contracted, is pressing against the bursa to hold the humeral head centered in the joint. Also, with too much inflammation, while supraspinatus is cushioned from bone below with the bursa, the confined bony space (the bony tunnel it passes through) can cause the muscle to scrape the underside of the acromion from above the muscle which is also painful.[10,25,28]
As discussed, the propensity for problems usually begins with an anatomical predisposition. Individuals with a more hooked acromion are at greater risk for impingement syndrome such as swimmers for example, due to repetitive overhand motions of the freestyle stroke.[3,4,6,8,14} X-ray and other imaging studies have demonstrated that those individuals with the acromial shape most likely to cause impingement in fact, suffer the most from the syndrome.[6,9,10,12,14,18,19,25,29,31,32]
Whether someone is born with an impingement prone condition or it develops over time is still a matter of debate; but clearly, the presence of a hooked acromion is found more commonly in those individuals with impingement syndrome.[13,23,24,33,35,36] The shape of the ligament connecting the acromion and the coracoid process can also influence the likelihood of impingement.[20}

An individual who has suffered with shoulder discomfort in the past during upper body work is very likely to continue to suffer unless modifications in their routine are employed.
Past trauma to the shoulder can also lead to bone spurs that will also increase the likelihood of or aggravate impingement, by reducing the space in that bony tunnel for supraspinatus and the bursa to move through.[11] Thus, there are many routes to creating the conditions for impingement syndromes. Once established, the chronic nature of inflammation and degenerative changes have a high probability of creating a state of ongoing trauma and further contributing to more inflammation and accelerating degenerative changes.
Thus, an individual who has suffered with shoulder discomfort in the past during upper body work is very likely to continue to suffer unless modifications in their routine are employed. There are several indications of potential a impingement syndrome.[2,7,11,21,22] One clue to either bursitis in this region or injury to the supraspinatus muscle itself is tenderness just below the acromion. Another clue to supraspinatus problems is pain during movements that increase the chance of impingement. Pain or discomfort during a movement while your shoulder is in an internally rotated position is also a tip-off. Simply put, routines with palms down will position the greater tuberosity in the best position for impingement. Overhand wide grip lat pulldowns can do this.
Also, performing a lateral side raise and pointing your thumb down near the top of the lift is most likely to produce impingement because the shoulder is internally rotated and positions the greater tuberosity optimally for impingement. Finally, shoulder pain at night during sleep can also be a subtle clue to minor irritation from impingement. If someone is anatomically predisposed to these problems, pain and discomfort is likely when traditional lifting routines are employed. This is not a problem that can be 'worked through' in the classical sense; modifications to technique are required.
If you're interested in more on this topic, look up exercises to strengthen the supraspinatus muscle. These exercises differ in form and style from common lifting routines. In addition, modifications from simple to extensive in standard lifting routines to employ for overall upper body work to reduce the likelihood of further aggravating suprapinatus is advisable.
References
- 1972. Cunningham's Textbook of Anatomy. Oxford University Press, London.
- Almekinders, L. C. 2001. Impingement syndrome. Clin. Sports Med. 20:491-504.
- Arroyo, J. S., S. J. Hershon, and L. U. Bigliani. 1997. Special considerations in the athletic throwing shoulder. Orthop. Clin. North Am. 28:69-78.
- Banas, M. P., R. J. Miller, and S. Totterman. 1995. Relationship between the lateral acromion angle and rotator cuff disease. J. Shoulder. Elbow. Surg. 4:454-461.
- Bigliani, L. U., R. Kelkar, E. L. Flatow, R. G. Pollock, and V. C. Mow. 1996. Glenohumeral stability. Biomechanical properties of passive and active stabilizers. Clin. Orthop.13-30.
- Bigliani, L. U., J. B. Ticker, E. L. Flatow, L. J. Soslowsky, and V. C. Mow. 1991. The relationship of acromial architecture to rotator cuff disease. Clin. Sports Med. 10:823-838.
- Brossmann, J., K. W. Preidler, R. A. Pedowitz, L. M. White, D. Trudell, and D. Resnick. 1996. Shoulder impingement syndrome: influence of shoulder position on rotator cuff impingement—an anatomic study. AJR Am. J. Roentgenol. 167:1511-1515.
- Cohen, R. B. and G. R. Williams, Jr. 1998. Impingement syndrome and rotator cuff disease as repetitive motion disorders. Clin. Orthop.95-101.
- Epstein, R. E., M. E. Schweitzer, B. G. Frieman, J. M. Fenlin, Jr., and D. G. Mitchell. 1993. Hooked acromion: prevalence on MR images of painful shoulders. Radiology 187:479-481.
- Farley, T. E., C. H. Neumann, L. S. Steinbach, and S. A. Petersen. 1994. The coracoacromial arch: MR evaluation and correlation with rotator cuff pathology. Skeletal Radiol. 23:641-645.
- Fongemie, A. E., D. D. Buss, and S. J. Rolnick. 1998. Management of shoulder impingement syndrome and rotator cuff tears. Am. Fam. Physician 57:667-2.
- Gagey, N., E. Ravaud, and J. P. Lassau. 1993. Anatomy of the acromial arch: correlation of anatomy and magnetic resonance imaging. Surg. Radiol. Anat. 15:63-70.
- Gill, T. J., E. McIrvin, M. S. Kocher, K. Homa, S. D. Mair, and R. J. Hawkins. 2002. The relative importance of acromial morphology and age with respect to rotator cuff pathology. J. Shoulder. Elbow. Surg. 11:327-330.
- Gohlke, F., T. Barthel, and A. Gandorfer. 1993. The influence of variations of the coracoacromial arch on the development of rotator cuff tears. Arch. Orthop. Trauma Surg. 113:28-32.
- Green, A. 1995. Arthroscopic treatment of impingement syndrome. Orthop. Clin. North Am. 26:631-641.
- Horrigan, J. and J. Robinson. 1991. The 7-Minute Rotator Cuff Solution. Health for Life, Los Angeles, CA.
- Humphreys, C. L. 1999. Shoulder Injuries & Weight Training. MuscleMag International, Mississauga, ON CA.
- Hyvonen, P., M. Paivansalo, H. Lehtiniemi, J. Leppilahti, and P. Jalovaara. 2001. Supraspinatus outlet view in the diagnosis of stages II and III impingement syndrome. Acta Radiol. 42:441-446.
- Kitay, G. S., J. P. Iannotti, G. R. Williams, T. Haygood, B. J. Kneeland, and J. Berlin. 1995. Roentgenographic assessment of acromial morphologic condition in rotator cuff impingement syndrome. J. Shoulder. Elbow. Surg. 4:441-448.
- Kopuz, C., S. Baris, M. Yildirim, and B. Gulman. 2002. Anatomic variations of the coracoacromial ligament in neonatal cadavers: a neonatal cadaver study. J. Pediatr. Orthop. B 11:350-354.
- Neer, C. S. 1972. Anterior acromioplasty for the chronic impingement syndrome in the shoulder: a preliminary report. J. Bone Joint Surg. Am. 54:41-50.
- Neer, C. S. 1983. Impingement lesions. Clin. Orthop.70-77.
- Nicholson, G. P., D. A. Goodman, E. L. Flatow, and L. U. Bigliani. 1996. The acromion: morphologic condition and age-related changes. A study of 420 scapulas. J. Shoulder. Elbow. Surg. 5:1-11.
- Pfahler, M., S. Haraida, C. Schulz, H. Anetzberger, H. J. Refior, G. S. Bauer, and L. U. Bigliani. 2003. Age-related changes of the glenoid labrum in normal shoulders. J. Shoulder. Elbow. Surg. 12:40-52.
- Prato, N., D. Peloso, A. Franconeri, G. Tegaldo, G. B. Ravera, E. Silvestri, and L. E. Derchi. 1998. The anterior tilt of the acromion: radiographic evaluation and correlation with shoulder diseases. Eur. Radiol. 8:1639-1646.
- Prescher, A. 2000. Anatomical basics, variations, and degenerative changes of the shoulder joint and shoulder girdle. Eur. J. Radiol. 35:88-102.
- Santavirta, S., Y. T. Konttinen, I. Antti-Poika, and D. Nordstrom. 1992. Inflammation of the subacromial bursa in chronic shoulder pain. Arch. Orthop. Trauma Surg. 111:336-340.
- Suenaga, N., A. Minami, K. Fukuda, and K. Kaneda. 2002. The correlation between bursoscopic and histologic findings of the acromion undersurface in patients with subacromial impingement syndrome. Arthroscopy 18:16-20.
- Toivonen, D. A., M. J. Tuite, and J. F. Orwin. 1995. Acromial structure and tears of the rotator cuff. J. Shoulder. Elbow. Surg. 4:376-383.
- Townsend, H., F. W. Jobe, M. Pink, and J. Perry. 1991. Electromyographic analysis of the glenohumeral muscles during a baseball rehabilitation program. Am. J. Sports Med. 19:264-272.
- Umans, H. R., H. Pavlov, M. Berkowitz, and R. F. Warren. 2001. Correlation of radiographic and arthroscopic findings with rotator cuff tears and degenerative joint disease. J. Shoulder. Elbow. Surg. 10:428-433.
- Wang, J. C., G. Horner, E. D. Brown, and M. S. Shapiro. 2000. The relationship between acromial morphology and conservative treatment of patients with impingement syndrome. Orthopedics 23:557-559.
- Wang, J. C. and M. S. Shapiro. 1997. Changes in acromial morphology with age. J. Shoulder. Elbow. Surg. 6:55-59.
- Wilk, K. E., C. A. Arrigo, and J. R. Andrews. 1997. Current concepts: the stabilizing structures of the glenohumeral joint. J. Orthop. Sports Phys. Ther. 25:364-379.
- Worland, R. L., D. Lee, C. G. Orozco, F. SozaRex, and J. Keenan. 2003. Correlation of age, acromial morphology, and rotator cuff tear pathology diagnosed by ultrasound in asymptomatic patients. J. South. Orthop. Assoc. 12:23-26.
- Yazici, M., C. Kopuz, and B. Gulman. 1995. Morphologic variants of acromion in neonatal cadavers. J. Pediatr. Orthop. 15:644-647.

